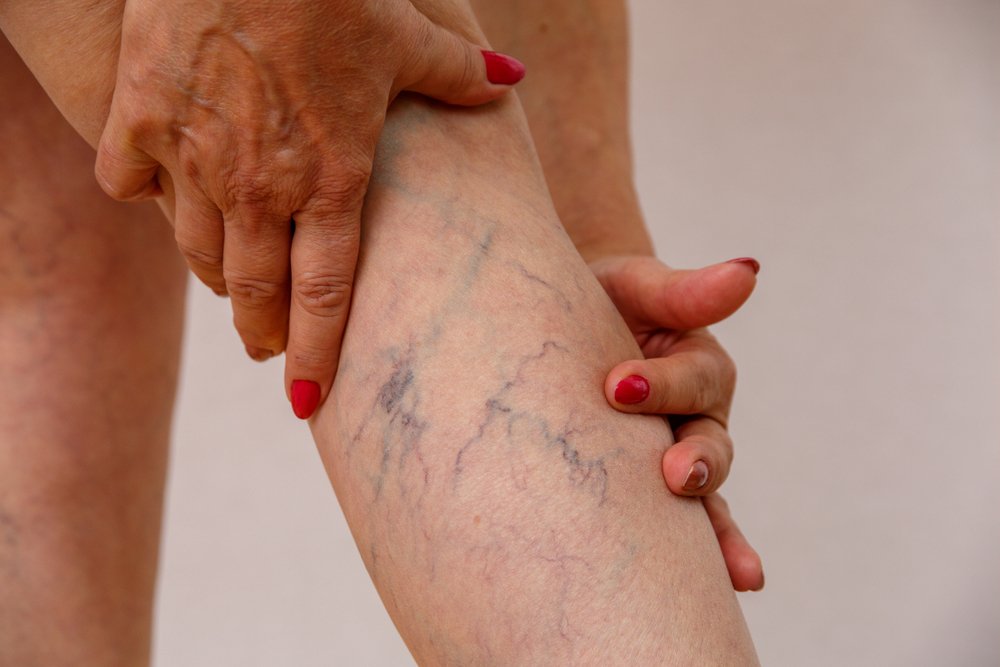
 When it comes to vascular health, the term 'varicose veins' strikes a peculiar mix of worry and curiosity. Characterized by twisted, bulging veins that are often purple or blue in color, varicose veins are not only a cosmetic concern but also a potential precursor to more severe conditions. One of the unsettling questions that arises around this topic is the possibility of varicose veins actually bursting. In this comprehensive exploration, we will unravel the reasons behind such concerns and the preventative measures every health-conscious individual should be aware of.
When it comes to vascular health, the term 'varicose veins' strikes a peculiar mix of worry and curiosity. Characterized by twisted, bulging veins that are often purple or blue in color, varicose veins are not only a cosmetic concern but also a potential precursor to more severe conditions. One of the unsettling questions that arises around this topic is the possibility of varicose veins actually bursting. In this comprehensive exploration, we will unravel the reasons behind such concerns and the preventative measures every health-conscious individual should be aware of.
The Anatomy of Varicose Veins
Varicose veins develop when small valves inside the veins stop functioning properly. They're responsible for keeping the blood flowing in one direction towards the heart. If these valves are weakened or damaged, blood may pool in your veins, causing them to become swollen and twisted over time. The most common location for varicose veins is in the legs and the feet, given the additional pressure placed on these veins due to standing and walking upright.
When the pressure in these veins becomes too high, there's a risk of the vein walls growing thinner and rupturing. This can occur from a minor trauma such as a bump or cut, or it can happen spontaneously if the pressure is consistently high.
Why and How Do Varicose Veins Burst?
The pressure inside a vein is normally much lower than the pressure in an artery. However, the pressure within varicose veins increases exponentially because these weakened vessels can't efficiently return blood to the heart. Imagine filling a balloon with more air than it can hold – that's the basic principle upon which varicose veins burst.
Various reasons can elevate this pressure, including:
Prolonged Standing or Sitting
Sedentary lifestyles or jobs that require long periods of standing can lead to stagnant blood in the lower leg veins. Over time, this can weaken the vein walls, making them prone to ruptures.
Pregnancy
The amount of blood in your body increases during pregnancy, but the blood flow from your legs to your pelvis decreases. This circulatory change can cause veins in your legs to become larger, increasing the pressure on the vein walls.
Obesity
Excess weight places additional and undue pressure on the veins, contributing to compromised vein health.
Lack of Exercise
Physical inactivity can lead to poor blood circulation, causing blood to pool in your veins.
Age
The wear and tear on vein valves over the years can cause them to malfunction and lead to varicose veins and potentially, vein ruptures.
Recognizing the Symptoms of Impending Rupture
Before varicose veins rupture, there are usually signs that the vein is under strain. Some of the symptoms to watch out for include:
Sudden Intense Pain
Prior to a vein bursting, you might experience a sudden and sharp pain along the course of the affected vein.
Swelling
The affected area may start to swell due to an accumulation of blood and fluids.
Visible Changes
The varicose vein may appear more twisted, enlarged, and prominent.
Skin Discoloration
The skin over the affected vein may become discolored, often presenting a reddish or bluish coloration due to the accumulation of deoxygenated blood.
Treatment and Prevention Strategies
Preventing varicose veins from reaching the point of rupture is essential for maintaining vascular health. Here are several strategies to consider:
Regular Exercise
Daily physical activity keeps your blood circulating through your legs and can work effectively to prevent varicose veins.
Watch Your Weight and Diet
Eating a low-salt, high-fiber diet ensures the prevention of swelling and supports the overall health of your circulatory system.
Elevate Your Legs
When resting or sleeping, elevate your legs above the level of your heart to assist in the circulation of blood back to your heart.
Avoid Prolonged Standing or Sitting
Take regular breaks to move around throughout the day, especially if your job requires long periods of sitting or standing.
Wear Compression Stockings
These can significantly reduce the discomfort associated with varicose veins and lower the risk of ruptures.
Medical Interventions
If your varicose veins are particularly painful or severe, there are a number of medical treatments available, from minimally invasive procedures like sclerotherapy and endovenous laser treatment (EVLT). Your healthcare provider, preferably a Board Certified Vascular Specialist can guide you to the most appropriate course of action.
Be vigilant in your observation of varicose veins and vigilant against their potential to burst. Understanding the causes and symptoms of varicose veins can help you make informed decisions about your health and take proactive measures to prevent any complications. Remember, while a burst varicose vein may be initially manageable, it's always best to avoid a situation that could lead to such a health scare. Take the necessary precautions for a safer and healthier future for your vascular system.
Want to have your Questions answered? Make an appointment with Dr. Gulshan Sethi; you can call at 516-606-7811 or click the link here.
